Combining robotics with virtual reality holds great promise for physical rehabilitation. Fixed frame, or stationary exoskeletons for the upper and lower body have been used for years to get patients moving again.
Introduction:
Rehabilitation exoskeleton devices provide power assistance to weakened limbs. The power assistance can be scaled back as the body part(s) gets stronger during the course of the rehabilitation program. Exoskeletons and other wearable robotic devices can guaranty that each movement is completed correctly and in exactly the same way. The number of repetitions with an exoskeleton (be it steps, or hand movements, etc…) is usually greater than classical rehabilitation. Furthermore, the wearable device can also be used to evaluate a patient’s mobility and the data for each user can be uploaded to a computer. Because these types of exoskeletons are stationary, the bulk of the electronics such as power supply, controllers, and cooling mechanisms can be positioned away from the user and the device doesn’t have to be compact.

The advantages of fixed/stationary frame exoskeletons, however, come at a price, the user will not leave their room while using them. Because the operators can’t roam about, they require at least a minimum level of stimulation and feedback in order to be engaged with the exercise program. Hocoma, a leader in stationary physical rehabilitation exoskeletons, conducted a webinar in February 2017 titled “Virtual Rehabilitation – How Feedback and Motivation Influence Therapy Outcome” that provided a great deal of clarity on this topic. Getting people invovled is key, according to the first guest speaker at the webinar, Dr. John Krakauer, Professor of Neurological and Neuroscience at Johns Hopkins University School of Medicine, U.S.
The potential of Virtual Reality (VR):
Here is how Dr. Krakauer describes the potential advantages of virtual reality: If we accept that as many as 40% of people in the U.S. have a gym membership that they don’t use why would people in need of medical rehabilitation be more motivated? In addition to rehabilitation being repetitive and boring, it reminds people of their deficiencies. And this is assuming a standard one to three hour rehabilitation session, but studies suggest sessions should go for four, five or even eight hours. How is anyone going to keep participants active and engaged for eight hours at a time? VR technology is not a solution to rehabilitation, but it can be a tool to keep people occupied, focused, and motivated.
Reward and motivation enhances learning. But that doesn’t mean taking a boring exercise and pretending that it is interesting. What VR could do is completely immerse the patient and provide them with an experience that they would not otherwise be able to have. The goal is to make the rehabilitation program several orders of magnitude more interesting.
A third advantage of VR rehabilitation was listed by the second guest speaker Martin Prins, Military Rehabilitation Center Aardenburg Doorn, Netherlands, Center of Excellence in Virtual Reality. Martin Prins, who has worked with various forms of rehabilitation with virtual reality starting in 2008, the users are more driven to overcome their limitations. VR patients tend to forget their own impairments. Professor Prin’s lab would sometimes show videos of what the patients are doing while using VR and they would be surprised by what they have achieved (think The King’s Speech). Of course, this works in reverse too, as some become too confident and emboldened.
A fourth advantage of VR for physical rehabilitation is the potential to make intuitive programs that do not require instructions. For example, keeping the spine straight could result in large rewards in the virtual world. Rather than having a physiotherapist remind you to keep a specific position, sensors on your body translate your body posture into consequences in the virtual world.
This is particularly useful for people with cognitive disability (example, speech complex damaged due to stroke). The participants can figure out what is desired of them within a few minutes without communication. There is no therapist pointing: “pick up this object.” It is the game design that rewards and teaches the user for executing the correct decisions. It can be played purely using trial and error learning.
Finally, another foreseen advantage to merging medical exoskeletons with VR is the ability for one rehabilitation professional to work with several patients at the same time. This becomes critical if daily rehabilitation does indeed need to be increased to eight hours per day.
All speakers agreed that VR holds advantages for superior feedback and transporting patients in any environment imaginable. There are no schools on how to become a VR rehabilitation doctor. But by implementing it, companies, labs and content designers can see where there are opportunities for new applications. There are many possibilities in the future. But we have to come up with new ideas about the experiences patients have in those realities.
An Example of digital feedback (not VR yet):
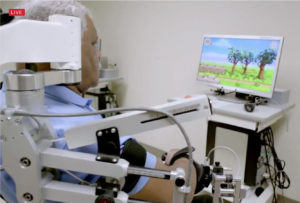
One success story of implementing physical rehabilitation with exoskeletons and virtual reality (or an earlier form of it at least) is the Armeo Power. The Armeo Power is a powered arm exoskeleton that provides additional force to resist gravity and facilitate arm movement. The goal is for patients to make a large number of movements early, for example after a stroke. Users can cover as much as one to two kilometers worth of arm movements while controlling a virtual dolphin. This is several times more than a regular rehabilitation session.
Limitations:
You may have noticed that nearly the entire article is based on “potential,” “may,” and “could.” Even if VR does deliver, it is going to be a piece of the puzzle for better healthcare, not the full solution. There are years of research ahead, and it is already known that some people can’t handle VR and feel sick when wearing the goggles (see Virtual Reality Sickness – Wikipedia). There is also not enough data at this point to prove that physical rehabilitation with exoskeletons and virtual reality is retained.
Sources & Information:
Special thanks to Dr. Clemens Müller from Hocoma for leading the webinar. You can find this and other Hocoma webinars at the Hocoma Academy: https://www.hocoma.com/services/hocoma-academy/











1 Comment